1. Introduction
Marcus Maurer, Petra Staubach
Urticaria
Urticaria (the medical term for hives) involves the sudden appearance of itchy wheals on the skin – on the entire body or just on one part of it, after certain stimuli (e.g. cold or sunlight), or the wheals may appear spontaneously, i.e. without any apparent particular reason (Ill. 1). In addition, many patients develop so-called angioedema, swelling of the skin or of the mucosa. In but a few patients only angioedema develop and no wheals. Nevertheless, this condition is also called urticaria.
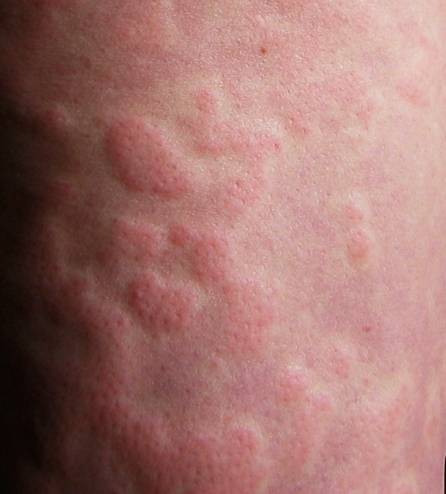
Illustration 1 Spontaneous urticaria wheals (Source: www.urtikaria.net)
Wheals
Wheals is the term used to describe the skin when it looks as if it has come into contact with stinging nettles. The name urticaria is derived from the nettle (lat. Urtica diocia or urtica urens, the common nettle), the reason surely, when urticarial, the skin looks as if it has been “stung” by stinging nettles (Ill. 3.).
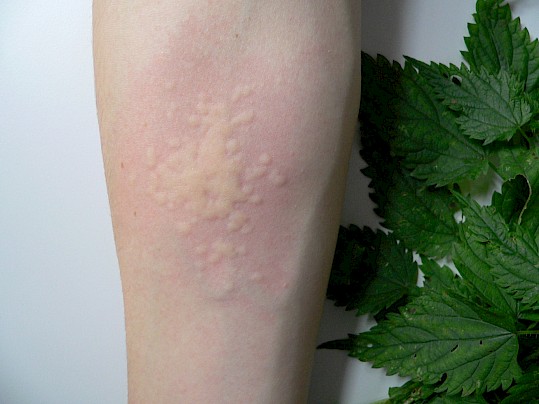
Illustration 3: The term “urticaria” is derived from stinging nettle (Urtica). (Source: Allergy Centre Charité)
Freshly developed wheals look like small whitish elevations on the skin, surrounded by a red flare. Wheals consist primarily of water released into the skin from the blood vessels. Thereby the smallest skin blood vessels are pressed together and can therefore transport only less blood; the skin then has a “whitish” appearance (Ill. 1a). 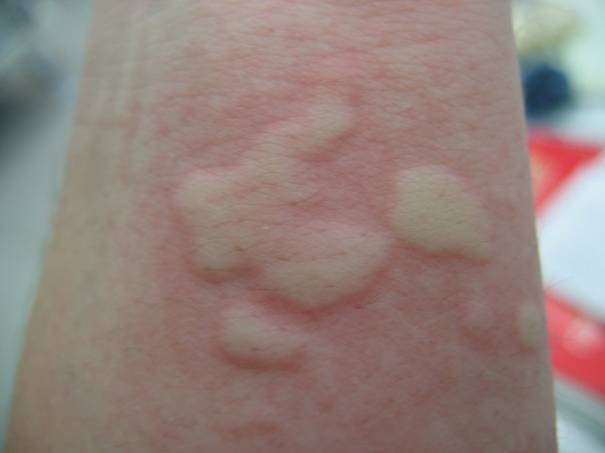
Illustration 1a Spontaneous urticaria wheals (Source: www.urtikaria.net)
We speak of the so-called giant wheals, when the wheals merge and spread over a large portion of the skin (Ill. 1b).
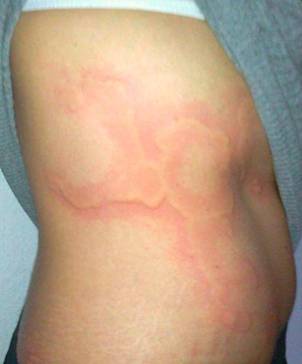
Illustration 1b Spontaneous urticaria wheals (Source: www.urtikaria.net)
The wheals need not always be whitish and the surrounding skin reddened, sometimes it is exactly the contrary. Particularly if the wheals last longer than a few hours they turn reddish-brown, while the flare around them decreases. The urticaria wheals persist for minutes up to hours, in the case of some patients – rarely – last even longer than one day. They disappear without leaving any visible secondary damage.
Angioedema
Put in simple terms, angioedema is a wheal in the deeper skin layers. While whealing results from fluid escaping from the blood vessels directly under the skin surface, in the case of angioedema the “leak” is deeper. The borders of swellings are therefore less visible and their colour is often not evidently different to that of normal skin. Angioedema frequently occur in the face, affect the hands and feet (Ill. 2).

Illustration 2: Outlined swelling on the left hand. Many patients, but not all urticaria patients, experience such angioedema. Exclusively such angioedema and no wheals are experienced by some patients with urticaria. Angioedema frequently occur in hands and feet and in the face. (Source: www.urtikaria.net)
Due to the particular composition of the skin, the swellings around the eyes and the lips are moderate to severe; however, these symptoms also manifest themselves in the genital area. Angioedema may persist for up to 2 days. Sometimes patients experience pain in the area affected by angioedema. There are other forms of angioedema, too which last longer than two days, the symptoms frequently occur in combination with gastrointestinal disorders or/and recur frequently as familial disposition. In the latter case further clarification should, by all means, be sought.
Pruritus
Beyond the fact that wheals and angioedema can lead to temporary, pronounced disfigurement, particularly in the face, itchiness is the greatest problem for patients with urticaria. Night itchiness can be especially distressful for patients suffering from urticaria; it robs them of their sleep. Itchiness is especially bad for those patients suffering from a special form of urticaria, the so-called symptomatic dermographism (also known as urticaria factitia). Scratching and rubbing the skin stimulates new wheals to develop and a further attack of itchiness – the onset of a vicious circle. The slightest stimulation of the skin, e.g. unconscious rubbing when asleep can give rise to bouts of itchiness. Patients then report they “scratched themselves raw”. It is extremely difficult to ignore pruritus/itchiness! Try for yourself not to scratch when you feel an itch somewhere (e.g. next time you are stung by a mosquito). Recurring itchiness can (as is the case in recurrent pain) become a tremendous burden and as consequence significantly diminish the quality of life.
25 Percent
Urticaria, also known as hives/nettle rash, is one of the most common skin diseases. Generally the definition “Urticaria” is given preference as it is an international term and the patients affected do not really have anything to do with nettles or wheals. About one in four people experience urticaria in the course of their lives. Most of these episodes last only for a few days or weeks and are uncomplicated. It is generally termed acute urticaria. Urticaria lasting for several months or years (sometimes decades) is much more difficult to endure and is then defined as chronic urticaria.
Urticaria – a typical women’s disease?
Almost all the studies into this issue reveal that women, do indeed, suffer more frequently from urticaria than men do. For chronic idiopathic urticaria, a ratio (women to men) of 2:1 has been revealed. Surprisingly this ratio does not hold true for children, i.e. girls suffer from the condition roughly as frequently as boys do, whereby little data is available in such connection. Why adult women develop chronic urticaria in higher numbers than adult men do has not been ascertained yet. It may reflect that the severity of this form of hives is frequently greater in women, lasts longer or that women are more inclined or prepared to consult a doctor for treatment. It is also interesting that men are more frequently affected by the inducible forms of urticaria, such as urticaria factitia; possibly because the symptoms associated involve particularly strenuous physical activity and are considered annoying.
Age and geographic distribution
Urticaria can break out at any age, from early infancy to old age. The age group of the 30 to 50-year-olds is the most frequently affected. First-time occurrences after 70 are rare. By contrast, hives that last only a few days are not uncommon in new-borns. Even in the case of worldwide distribution, this disease is not choosy. Urticaria is known on all the continents.
Figures and facts relating to hives
Urticaria is a particularly common disease. It is estimated that one in four people experiences urticaria at least once in their lives. This generally involves acute urticaria. According to conservative estimates currently 1 in 100 suffers from chronic urticaria. Data on average durations of the disease are rare and often contradictory (urticaria is a very unpredictable disease). Frequently chronic urticaria lasts several years. Some patients report about decades with the disorder. Individualised predictions are not possible. It is important to know that chronic urticaria disappears at some time or the other in all patients. This means urticaria appears spontaneously and very frequently disappears spontaneously. Contrary to neurodermatitis or psoriasis the disposition to develop this disease is not inherited.
Trigger
Many substances can trigger wheals and itchiness. Many of these substances are produced by the body itself and act on the skin “from inside”. However, there are numerous substances in our environment that cause our skin to itch and wheal. A common characteristic of most of these substances is that they release the messenger histamine, believed to play a key role in triggering wheals, itching and angioedema. This itch-triggering effect of histamine is very clearly evident after an insect bite for example, or after contact with stinging nettles. Beyond substances that release the body’s supply of histamine, the venom of many insects and pruritic (itch-inducing) plants contains histamine that penetrates and stimulates the skin. The stimulant is sensed by specialised nerves (one might also say the “itch nerves”). A message is sent to the brain, the neural circuitry of the brain: something is itching here! This is often quite a good thing. In the case of insect bites or following contact with pruritic plants, itchiness induces us to scratch the skin, cool it under cold water (and thereby eliminate the trigger) or rub it (whereby more blood reaches the spot of the reaction allowing the itch stimulants or venoms to be transported away more quickly with the bloodstream). Almost all of the histamine is stored in a specific kind of cell, the so-called mast cells. When these cells are activated, i.e. if they are “nettled” by a stimulant (and there are a number of stimulants that do so), the mast cells release their histamine into the skin tissue resulting in whealing and itching.
Mast cells as key cells of urticaria
One process is common to all forms of urticaria. Histamine (Ill. 4) and many other inflammation triggers, e.g. leukotrienes or the platelet activating factor (PAF) is released by activating mast cells in the skin.
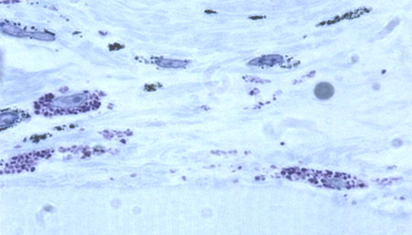
Illustration 4: Mast cells (dark blue) – the cells which trigger urticaria symptoms. (Source: Allergy Centre Charité)
These factors then lead to the dilation of the blood vessels in the skin followed by swelling and itching. Mast cells are actually the “firefighters” or the “border patrol” of the human body. They are most commonly found in the parts of the body where we have direct contract with our environment: in the skin, in the mucous membranes of the gastrointestinal tract and in the respiratory tract. They fulfil crucial life functions for the body: dangerous assailants like bacteria or parasites are identified and neutralised – be it because the mast cells block the path of the intruders into the body, neutralise their venom, because they kill or eat them, or because they alarm the cells of the immune system (our body’s defence system) and direct them to the spot of the incidence.
The prevalence of mast cells in the skin and in the mucous membranes of the human body explains why urticaria is particularly noticeable in those spots. The activation of the mast cells in the upper (outermost) dermal and mucous membrane layers leads to wheals, while the activation in the lower (deeper) dermal layers leads to deeper swelling (angioedema). An activation of the mast cells in the mucous membranes of the pharynx and of the respiratory tract can lead to difficulty in swallowing and create respiratory distress; an activation of the mucous membranes of the gastrointestinal tract leads to stomach aches, nausea and diarrhoea.
Wheals and angioedema develop by the smallest skin vessels “leaking” in the area in which the skin is affected. The space between the cells that form the walls of the blood vessels increases, allowing blood plasma and other blood cells to escape from the interior of the blood vessels into the surrounding tissues. Apart from histamine, leukotrienes, PAF and other mast cell products increase the permeability of blood vessels. The fact that antipruritic substances are, in many cases, effective in connection with urticaria may be explained by the fact that these drugs directly block the impact of histamine. These drugs are therefore also called antihistaminic drugs. Antihistaminic drugs have been tested and proven for decades. They are generally tolerated very well; serious side effects are extremely rare. Formerly antihistaminic drugs often made the patient very tired. In the modern antihistaminic drugs of the 2nd generation this adverse effect has been more or less “eliminated”. When “antihistaminic drugs” are spoken of in the following text, the modern antihistaminic drugs of the 2nd generation which do not cause drowsiness are meant. The fact that antihistaminic drugs are not always effective for all cases of urticaria indicates that histamine is not the only substance which triggers itchiness and wheals.
Appearance of the skin
Urticaria typically involves the greatly changing appearance of the skin which many patients describe as follows time and again: “In the evening my skin is completely normal, next morning it looks like a piece of crumble, the itchiness is hardly bearable and by the time I finally get to the doctor in the late morning, it has disappeared”. Wheals usually appear daily, may, however, also appear less frequently with symptom-free intervals. During a bout wheals can most frequently be detected, however also flares and deep skin swellings (angioedema) are not uncommon. 50 % of the patients with urticaria get both wheals and angioedema. About 40 % of the patients with urticaria only experience wheals, less than 10 % only angioedema. It is not known yet why urticaria frequently lasts longer and takes a more severe course in patients who also have angioedema.
Symptoms
The worst for urticaria patients is the often unbearable itchiness that is experienced as a torture. When we think about being touched at just one spot or are stung by a mosquito, we can think of nothing else but the itchiness in such connection it is understandable that patients suffering from this itchiness for days, months and years all over the body, almost “go mad” and have lost their quality of life. In addition, the human body has difficulty to adapt to itchiness – contrary to other stimulants such as, for instance heat or pressure. The itchiness in the case of hives by the way calls for a rub (unlike to the itchiness associated, for example, with neurodermatitis). i.e. skin scratched by fingernails is rarely found. On the contrary, it is often reported that the itchy spots of the skin have to be “rubbed” with the fingertips for a long time. The affected spots are frequently perceived as hot, after the episode dies down – as dry. Sometimes patients also speak of the skin burning, or downright pain in case of angioedema in the affected skin (Ill. 5).
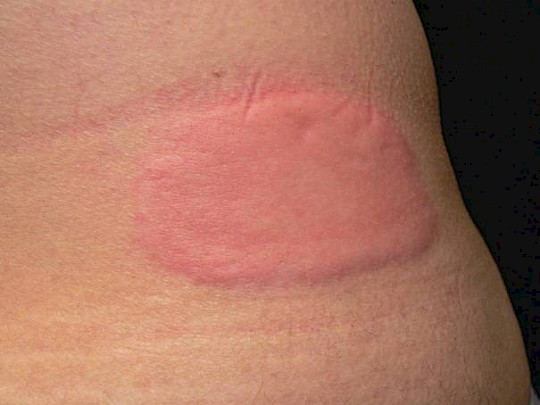
Illustration 5: Occasionally wheals can burn or be painful. (Source: Allergy Centre Charité)
Further symptoms
Many patients complain of headaches or joint pain during an episode of urticaria. The first thing to be determined is whether the wheals, itchiness and swelling are the result of pain treatment and whether they were triggered by the ingestion of acetylsalicylic acid (ASS, e.g. in Aspirin®), or other chemically related drugs (e.g. Diclofenac, Ibuprofen) – many drugs are known to induce urticaria or to trigger urticaria (see Section “Acute spontaneous urticaria”). Patients suffering from urticaria should take another pain killer, e.g. Paracetamol instead of acetylsalicylic acid, Diclofenac or Ibuprofen. However, pain may also indicate an infection. It is known that chronic infections, i.e. those that persist of a longer period in the body and which do not directly show symptoms, may support urticaria. Headaches and joint pains, may, however trigger symptoms of urticaria, possibly due to the release of high quantities of histamine and other substances.
Similar clinical pictures
It is actually fairly difficult to confuse urticaria with other diseases. This reflects the highly characteristic skin manifestations associated with urticaria; the wheal and flare-type skin reaction and the swelling of the skin’s deep tissue. These manifestations are also transient, i.e. only last for a short period (wheals: minutes to a few hours, angioedema: hours to a few days). Wheals and angioedema heal without leaving any visible traces on the skin. There are neither scars nor scabs, nor haemorrhaging. This already clearly differentiates urticaria from most other skin diseases. In other words; if the characteristic itchiness appears together with the wheal and/or swelling, then the diagnosis of urticaria is an easy one. Nevertheless, a thought must be spent on the idea that other diseases than urticaria may at times give rise to the appearance of wheals and/or angioedema.
If exclusively recurrent angioedema (without wheals) appear, these may be caused by taking a high blood pressure drug (particularly ACE inhibitors), very rarely even hereditary diseases, the typical symptoms of which are angioedema, e.g. a hereditary angioedema (HAE). Here too, swelling of the skin appears, particularly in the face. Most of the patients with HAE also suffer from very painful angioedema in the abdomen. These angioedema are not triggered by histamine, therefore do not respond to antihistaminic drugs, their symptoms are severer and last longer. Itching is, however, not involved at all. If exclusively recurrent itching wheals (but no angioedema) appear, the cause may be an autoinflammatory syndrome, whereby this is very rarely the case. Autoinflammatory syndromes are easy to determine by simple tests and can, as a rule, be treated effectively. Furthermore, urticaria-vasculitis, also a very rare disease, may be the cause for recurrent bouts of wheals. In the case of urticaria vasculitis the rather burning than itching wheals remain for more than a day and after they have healed may leave a brownish stain. Wheals may, however, be combined with other symptoms such as blisters. In all these so-called differential diagnoses further clarification should be sought by consulting a doctor/dermatologist.
Urticaria is classified according to two different aspects. First and foremost, classification is according to the duration in acute (lasting less than 6 weeks) and chronic (lasting more than 6 weeks). The chronic form is further classified in chronic spontaneous urticaria and chronic inducible urticaria. Urticaria is always inducible when the wheals can be specifically triggered. In the case of a physical urticaria, the largest group of inducible urticaria, it can be induced by physical stimuli, such as, for instance heat, cold, light or pressure. The impact of this stimulant on the skin then leads to the appearance of wheals. In the case of contact urticaria, a further form of inducible urticaria, the contact of the skin with certain substances leads to the appearance of local wheals, for instance by touching stinging nettles or by coming into contact with a material you have an allergic reaction to. As the wheals are limited to the area of the skin which comes into contact with the stimulant, the distribution of the wheals is not incidental; they often form patterns which indicate the trigger. For instance in the case of solar urticaria, the wheals only appear on the light-exposed area while the areas not exposed to light and directly surround are absolutely free of symptoms. In the case of cholinergic urticaria, a frequent form of inducible urticaria, an increase in core body temperature triggers the development of wheals, whereby it is irrelevant whether the increase in body temperature was due to physical strain or, for instance, a hot bath. All inducible forms can also appear in combination with spontaneous urticaria.
Contrary to the inducible forms just brought forward, wheals develop “out of the blue” in the spontaneous form. The skin lesions appear beyond the control of the patient and on all possible areas of the skin, the borders of the hives are purely coincidental. Stress and heat may favour the development however, they are not really necessary for the symptoms to appear. The clearly most frequent form is acute spontaneous urticaria. About one in four people is affected at some time during life. Luckily the symptoms disappear again in the vast majority of cases in a few days or weeks. It is generally termed acute urticaria. If the symptoms last longer than 6 weeks it is termed chronic urticaria. This urticaria can last for several months or years (sometimes decades). This fact alone justifies the high number of patients
The majority of the patients suffering from chronic urticaria suffer from chronic spontaneous urticaria. The inducible forms of urticaria are less frequent. In this group most of the patients suffer from symptomatic dermographism (also urticaria factitia) or from cold urticaria. Aquagenic urticaria (triggered by water) or vibration-induced angioedema are absolute “rarities”. All the forms of urticaria are listed in the following table according to their classification.
Acute | Chronic | Chronic |
Acute, spontaneous urticaria | Chronic spontaneous urticaria | Chronic inducible urticaria |
| Spontaneous appearance of wheals, angioedema or both for less than 6 weeks for known and unknown causes | Spontaneous appearance of wheals, angioedema or both for more than 6 weeks for known and unknown causes | Physical urticaria
Contact urticaria (frequent) Aquagenic urticaria (very rare) 1also called urticaria factitia or demographic urticaria, |
Back to overview.






 English
English Deutsch
Deutsch Francais
Francais Español
Español



